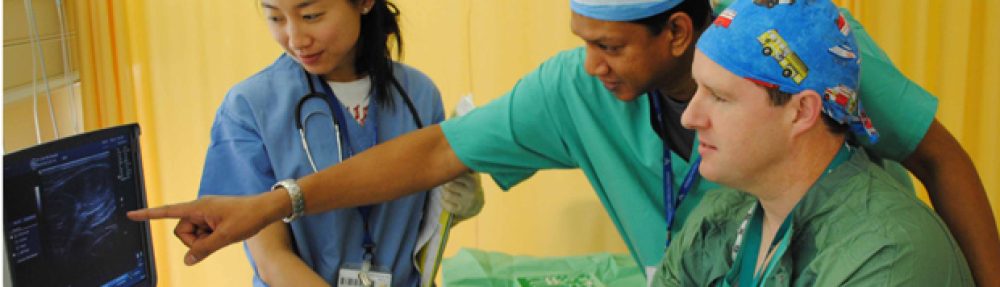
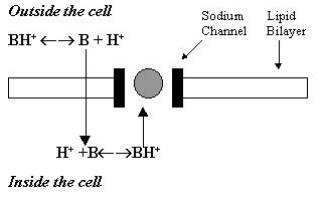
The ASA has issued guidelines for acute pain management in the perioperative setting. Click on this link to read guidelines. Obviously there is a North American flavour to these guidelines, but they are generalisable.
Summary:
1. Institutional Policies and Procedures for Providing Perioperative Pain Management
- Anaesthetists offering perioperative analgesia services should provide ongoing education and training to ensure that hospital personnel are knowledgeable and skilled with regard to the effective and safe use of the available treatment options within the institution.
- Educational content should range from basic bedside pain assessment to sophisticated pain management techniques (e.g., epidural analgesia, PCA, and various regional anesthesia techniques) and non-pharmacologic techniques (e.g., relaxation, imagery, hypnotic methods – these are US guidelines!).
- For optimal pain management, ongoing education and training are essential for new personnel, to maintain skills, and whenever therapeutic approaches are modified.
- Anaesthetists and other healthcare providers should use standardized, validated instruments to facilitate the regular evaluation and documentation of pain intensity, the effects of pain therapy, and side effects caused by the therapy.
- Anaesthetists responsible for perioperative analgesia should be available at all times to consult with ward nurses, surgeons, or other involved physicians.
- They should assist in evaluating patients who are experiencing problems with any aspect of perioperative pain relief.
- Anaesthetists providing perioperative analgesia services should do so within the framework of an Acute Pain Service.
- They should participate in developing standardized institutional policies and procedures.
2. Preoperative Evaluation of the Patient
- A directed pain history, a directed physical examination, and a pain control plan should be included in the anaesthetic preoperative evaluation.
3. Preoperative Preparation of the Patient
- Patient preparation for perioperative pain management should include appropriate adjustments or continuation of medications to avert an abstinence syndrome, treatment of preexistent pain, or preoperative initiation of therapy for postoperative pain management.
- Anaesthetists offering perioperative analgesia services should provide, in collaboration with others as appropriate, patient and family education regarding their important roles in achieving comfort, reporting pain, and in proper use of the recommended analgesic methods.
- Common misconceptions that overestimate the risk of adverse effects and addiction should be dispelled.
- Patient education for optimal use of PCA and other sophisticated methods, such as patient-controlled epidural analgesia, might include discussion of these analgesic methods at the time of the preanaesthetic evaluation, brochures and videotapes to educate patients about therapeutic options, and discussion at the bedside during postoperative visits.
- Such education may also include instruction in behavioral modalities for control of pain and anxiety.
4. Perioperative Techniques for Pain Management
- Anaesthetists who manage perioperative pain should use therapeutic options such as epidural or intrathecal opioids, systemic opioid PCA, and regional techniques after thoughtfully considering the risks and benefits for the individual patient.
- These modalities should be used in preference to intramuscular opioids ordered “as needed.”
- The therapy selected should reflect the individual anesthesiologist’s expertise, as well as the capacity for safe application of the modality in each practice setting.
- This capacity includes the ability to recognize and treat adverse effects that emerge after initiation of therapy.
- Special caution should be taken when continuous infusion modalities are used because drug accumulation may contribute to adverse events.
5. Multimodal Analgesia
- Whenever possible, anaesthetists should use multimodal pain management therapy.
- Unless contraindicated, patients should receive an around-the-clock regimen of NSAIDs or paracetamol.
- Regional blockade with local anaesthetics should be considered.
- Dosing regimens should be administered to optimize efficacy while minimizing the risk of adverse events.
- The choice of medication, dose, route, and duration of therapy should be individualized.
6. Patient Subpopulations
Paediatric patients
- Aggressive and proactive pain management is necessary to overcome the historic under-treatment of pain in children.
- Perioperative care for children undergoing painful procedures or surgery requires developmentally appropriate pain assessment and therapy.
- Analgesic therapy should depend upon age, weight, and comorbidity, and unless contraindicated should involve a multimodal approach.
- Behavioral techniques, especially important in addressing the emotional component of pain, should be applied whenever feasible.
- Sedative, analgesic, and local anaesthetics are all important components of appropriate analgesic regimens for painful procedures.
- Because many analgesic medications are synergistic with sedating agents, it is imperative that appropriate monitoring be used during the procedure and recovery.
Geriatric patients
- Pain assessment and therapy should be integrated into the perioperative care of geriatric patients.
- Pain assessment tools appropriate to a patient’s cognitive abilities should be used. Extensive and proactive evaluation and questioning may be necessary to overcome barriers that hinder communication regarding unrelieved pain.
- Anaesthetists should recognize that geriatric patients may respond differently than younger patients to pain and analgesic medications, often because of comorbidity.
- Vigilant dose titration is necessary to ensure adequate treatment while avoiding adverse effects such as somnolence in this vulnerable group, who are often taking other medications (including alternative and complementary agents).
Other subpopulations
- Anaesthetists should recognize that patients who are critically ill, cognitively impaired, or have communication difficulties may require additional interventions to ensure optimal perioperative pain.management.
- Anaesthetists should consider a therapeutic trial of an analgesic in patients with increased blood pressure and heart rate or agitated behavior when causes other than pain have been excluded.